Symptom Monitoring in California Hospice Care

Symptom monitoring in California hospice: a guide for families
TL;DR:
- Active symptom monitoring by families is essential for managing pain and breathlessness in hospice.
- Families should regularly track, report, and record symptom changes to inform care adjustments.
- Trust and partnership between families and healthcare providers enhance symptom management effectiveness.
Many families enter hospice care believing that comfort will simply arrive on its own. That is a natural assumption, but it misses something important. Up to 70% of dying patients experience treatable symptoms like pain and dyspnea (shortness of breath), and those symptoms require active, consistent attention to manage well. Hospice at home in California is not a passive experience. It is a carefully coordinated process where your observations as a caregiver carry real weight. This guide explains what symptom monitoring looks like in practice, which signs to watch for, and how to work with your hospice team to keep your loved one as comfortable as possible.
Table of Contents
- Why active symptom monitoring matters in hospice care
- Core symptoms to monitor: what to watch for and how
- The role of nursing staff, family logs, and follow-ups
- Practical strategies for managing pain and breathlessness
- A nuanced approach: what most guides miss about symptom monitoring
- Get guidance and support for symptom monitoring in California
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Active monitoring is essential | Tracking symptoms like pain and breathlessness daily keeps your loved one more comfortable. |
| Use simple tools and logs | Basic scales and a daily journal can help both family and nurses catch important changes early. |
| Teamwork improves care | Families and hospice staff work together, using communication and logs for faster adjustment to needs. |
| Mix care strategies | Both medications and comfort techniques like positioning work best when combined for symptom relief. |
| Human presence matters most | Your attention, observations, and compassion are just as vital as medical protocols for comfort at home. |
Why active symptom monitoring matters in hospice care
Hospice care is built around a clear purpose: comfort, not cure. Under California’s Medi-Cal program, hospice is certified in defined periods, specifically 90-day and 60-day benefit periods, each requiring physician oversight and a documented focus on symptom alleviation. That structure matters because it means every visit, every assessment, and every care plan adjustment is anchored to keeping your loved one comfortable during life’s final chapter.
Within that framework, family caregivers are not bystanders. You are active members of the care team. Hospice nurses typically visit several times a week, but you are present every day. That means your eyes, your instincts, and your notes fill in the gaps between professional visits in ways that no monitoring tool can replicate.
“The family caregiver is often the first to notice a subtle change in breathing, a shift in restlessness, or a new reluctance to eat. Those early observations are not minor details. They are clinical signals that help the entire team respond faster and more precisely.”
Symptom monitoring in hospice care involves three core actions: consistent tracking, timely reporting, and honest feedback. When you log what you see and share it clearly with the nursing team, you help them adjust medications, positioning, and comfort routines before a small problem grows into significant distress.
For a broader overview of how home-based care supports families through this process, the compassionate at-home support guide from Graceland is a helpful starting point.
Key principles of active symptom monitoring:
- Track symptoms at regular intervals, ideally at the same times each day
- Record changes in pattern, not just the symptom itself (for example, “pain was worse after repositioning”)
- Report anything that feels different from the day before, even if you are unsure it is significant
- Ask the nursing team what specific changes they want you to watch for
Pro Tip: Keep a simple notebook by the bedside labeled with the date each day. Write down pain levels on a 0 to 10 scale, breathing quality, appetite, sleep, and mood. This daily log becomes the most useful tool the hospice team has between visits, and it also gives you hospice care standards context for comparing notes with the clinical team.
Core symptoms to monitor: what to watch for and how
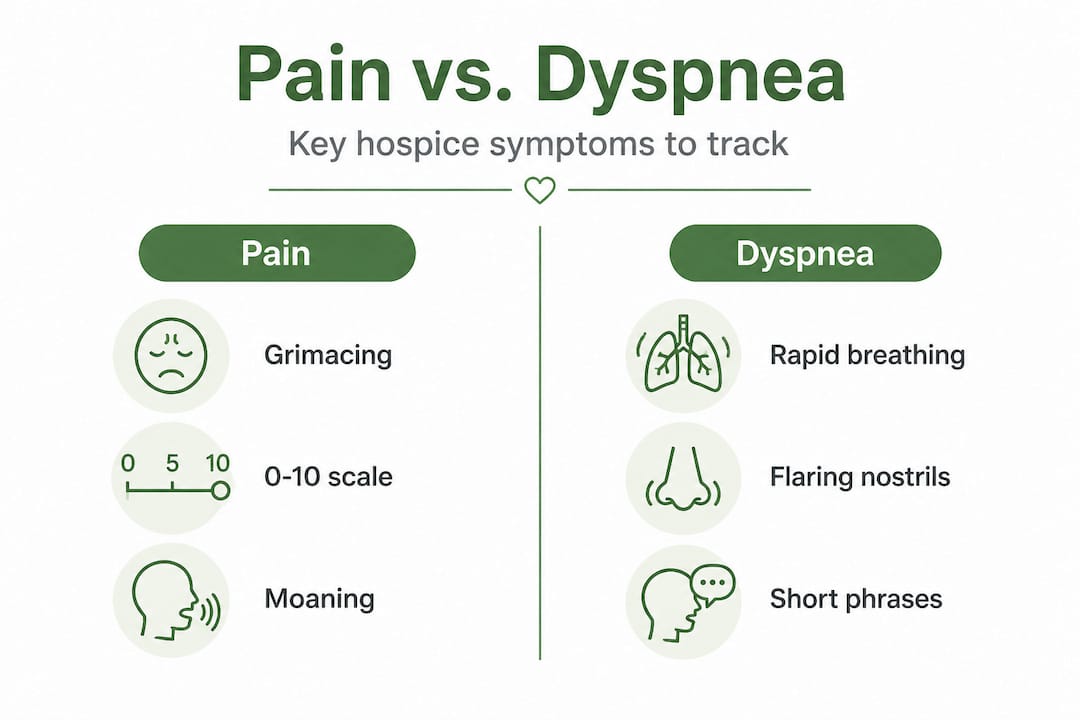
Once you understand why symptom monitoring matters, the next step is knowing what to look for. Two symptoms stand out above all others in hospice care: pain and dyspnea.
Pain affects approximately 70% of hospice patients, and dyspnea affects a similarly high proportion. Both can be measured at home with simple tools, even when the patient cannot speak clearly. Pain is not only physical. It can be emotional, spiritual, or relational, and a good monitoring approach pays attention to all of those dimensions.

For pain, the Edmonton Symptom Assessment System Revised (ESAS-r) offers a straightforward scale covering multiple symptoms at once. A simple 0-to-10 pain scale also works well. Zero means no pain, ten means the worst imaginable pain. When your loved one cannot self-report, watch for physical signs: grimacing, guarding a body part, resisting being touched, or changes in breathing when moved.
For dyspnea, nurses use a tool called the Respiratory Distress Observation Scale, or RDOS. You can watch for similar signs at home: rapid or shallow breathing, visible effort in the chest and neck muscles when inhaling, a look of distress or anxiety during breathing, and noisy or irregular breath sounds. These observations are worth writing down with the time they occurred. The HOPE Guidance Manual requires formal screening for both pain and non-pain symptoms at admission and at scheduled follow-ups, so your daily notes align directly with what the clinical team needs.
For more detailed guidance on managing these specific symptoms, the pain and symptom management resource from Graceland covers both medication and non-medication approaches in practical detail.
Common symptoms and how to monitor them at home:
| Symptom | What to observe | When to report |
|---|---|---|
| Pain | Facial expressions, body tension, pain scale rating | Score of 4 or higher, or sudden increase |
| Dyspnea | Breathing rate, visible effort, restlessness | Rapid breathing over 25 breaths per minute, distress |
| Nausea | Refusal to eat, retching, complaints | Persistent episodes lasting more than an hour |
| Agitation | Restlessness, calling out, inability to settle | Sudden onset or worsening overnight |
| Fatigue | Sleep duration, responsiveness, engagement | Sudden excessive sedation or unresponsiveness |
| Appetite changes | Food and fluid intake | Complete refusal to eat or drink for 24 hours |
Other symptoms worth watching include nausea, constipation, agitation, and changes in consciousness. Each one can usually be addressed with the right intervention once it is identified. For a full list of what hospice services can address, visit common hospice services to see what professional support looks like in practice.
Pro Tip: When your loved one cannot speak, your written observations become their voice. Document not just the symptom but what seemed to trigger it, what made it better, and how long it lasted. That context helps the nursing team decide whether to adjust medications or try a different positioning strategy.
The role of nursing staff, family logs, and follow-ups
Good symptom monitoring is a two-part process. Your family logs and the nursing team’s clinical assessments work together as a system, each providing information the other cannot.
The HOPE (Hospice Outcomes and Patient Evaluation) tool is a structured assessment used by hospice professionals to screen for pain and other symptoms at key points in care. When moderate to severe symptoms are reported, the HOPE protocol triggers a follow-up nursing visit within two days. That means your daily log does not just sit in a notebook. It can directly initiate a clinical response.
Here is how the process typically works in practice:
- You observe a change. For example, your loved one seems more uncomfortable than usual, rating their pain at a 6 when it has been a 3 all week.
- You log the change. Write down the time, the symptom, the intensity, and any possible triggers.
- You contact the hospice team. Call the nurse line to report the change, sharing what you observed and what your log shows.
- The nurse assesses the report. If the symptom is moderate to severe, a follow-up visit is scheduled promptly.
- The care plan is adjusted. Based on the combined clinical assessment and your notes, the team may change medications, add comfort measures, or modify routines.
- You receive updated guidance. The nurse explains what to watch for next and how to respond if symptoms worsen again.
This cycle of observation, reporting, and response is what makes home-based hospice effective. The hospice nurse responsibilities resource provides a clearer picture of exactly what nursing staff are trained to evaluate and how they use your input.
| What family logs cover | What professional assessment covers |
|---|---|
| Day-to-day symptom patterns | Clinical interpretation of symptoms |
| Changes in behavior or mood | Medication review and dosage decisions |
| What helped or made things worse | Physical examination findings |
| Food and fluid intake | Formal scoring using validated tools |
| Sleep and restlessness patterns | Care plan adjustments and documentation |
For a closer look at how the nursing visit itself is structured, the hospice visit workflow guide offers a step-by-step picture of what happens during each home visit.
Pro Tip: Write down not only the symptoms themselves but also what seemed to help and what made things worse. A note like “pain decreased after repositioning to the left side” is far more useful to the nurse than a simple pain score, because it points directly toward a non-medication comfort strategy that already works.
Practical strategies for managing pain and breathlessness
Knowing what to watch for and how to report it is essential. Knowing how to respond in the moment is equally important.
Both medication and non-medication approaches are effective at relieving pain and dyspnea in hospice care. Opioids, such as morphine and hydromorphone, are commonly prescribed for both symptoms. Many families feel hesitant about opioid use, which is completely understandable. The hospice team will guide you on dosing, timing, and what to watch for. When used correctly under professional supervision, these medications reduce suffering without hastening death.
Non-medication strategies are equally valuable and can often be used alongside medications. Research shows that up to 70% of patients benefit from combining both approaches, which is why your role in trying comfort measures at home matters so much.
Practical comfort strategies for pain and breathlessness:
- Repositioning: Gently shifting your loved one’s position every two hours relieves pressure, reduces localized pain, and can ease breathing. A slight elevation of the head of the bed often helps with both breathlessness and comfort.
- Cool airflow: A small fan directed near the face or an open window can significantly reduce the sensation of breathlessness. This works even when oxygen levels appear normal, because the sensation of moving air calms the brain’s response to dyspnea.
- Calm environment: Reducing noise, dimming lights, and speaking in a soft, steady voice all lower anxiety, which in turn reduces the body’s experience of pain and breathing difficulty.
- Gentle touch: Holding a hand, light massage, or simply sitting close communicates safety and reduces distress in ways that medications cannot.
- Breathing guidance: Slow, paced breathing encouraged by a calm caregiver voice helps regulate the patient’s own breathing rhythm, especially during moments of heightened breathlessness.
“Presence is a form of care. Sitting beside someone, speaking gently, and responding to their discomfort without rushing communicates something no medication can: that they are not alone.”
If symptoms feel uncontrolled between nursing visits, contact your hospice team right away. Do not wait for the next scheduled visit. The care team is available around the clock precisely for these moments. For additional comfort approaches you may not have considered, visit complementary hospice strategies for practical ideas that can be combined with medical care.
A nuanced approach: what most guides miss about symptom monitoring
Most resources on hospice symptom monitoring focus on tools and scales. The ESAS-r, the RDOS, the HOPE tool. These are genuinely useful, and we encourage every family to learn them. But it is important to say clearly: tools do not provide care. People do.
The most attentive caregiver is someone who has learned to read their loved one. Not through a checklist, but through years of shared experience. They know that a particular silence means discomfort. They notice the small frown that appears before a pain score would even register on a scale. Caregiver observations remain indispensable to effective hospice care, even as clinical tools improve.
There is also an emotional dimension to caregiving that rarely appears in monitoring guides. Watching someone you love struggle with pain or breathlessness is genuinely hard. It is exhausting, grief-laden, and sometimes frightening. That labor is real, and it deserves acknowledgment. Caregivers who feel supported and informed do a better job of monitoring because they are less overwhelmed. Supporting the caregiver is not separate from supporting the patient. It is part of the same effort.
The best outcomes in home-based hospice happen when families and clinical teams genuinely trust each other and learn from each other, rather than simply exchanging data. A nurse who listens carefully to a family’s intuition, and a family who trusts the nurse’s clinical judgment, create a partnership that no protocol alone can produce. That partnership is what turns symptom monitoring from a task into an act of love.
Get guidance and support for symptom monitoring in California
At Graceland Hospice, we understand that symptom monitoring can feel like a heavy responsibility, especially when you are already carrying the emotional weight of caring for someone you love. Our California-based hospice team is here to walk alongside you, offering expert guidance, hands-on support, and compassionate education for every family we serve.
Our comprehensive hospice offerings include skilled nursing visits, symptom management planning, caregiver education, and around-the-clock access to clinical support. We believe every eligible patient and family deserves the full benefit of hospice care, not just the medical components, but the human ones too. Contact us today for a free consultation and find out how we can help your family navigate this journey with confidence, clarity, and care.
Frequently asked questions
What symptoms are most important to monitor in hospice care?
Pain and shortness of breath are the most common and urgent symptoms to monitor, as both affect up to 70% of hospice patients and respond well to timely intervention.
How often should families update hospice staff about symptoms?
Families should report changes as they happen, and formally notify the team when symptoms become moderate or severe, since the HOPE protocol requires follow-up within two days of such reports.
What can families do if symptoms get worse between hospice visits?
Contact the hospice team immediately using the 24-hour nurse line, and share your symptom log so the team can arrange a timely RN follow-up and adjust the care plan as needed.
Are non-medication options effective for managing pain or breathlessness at home?
Yes. Positioning, cool airflow, and calming presence are all clinically recognized comfort strategies that often work best when combined with prescribed medications.
Who is responsible for tracking symptoms in California hospice care at home?
Both family caregivers and the hospice nursing staff share responsibility, and the HOPE tool is designed to coordinate those two streams of information into a unified, responsive care plan.
Recommended
- Understanding Hospice Care Levels: A Guide for California Families | Graceland Hospice Care Blog
- Emergency care in hospice: a guide for California families | Graceland Hospice Care Blog
- Answers to common hospice questions: a California family guide | Graceland Hospice Care Blog
- Blog & Resources | Graceland Hospice Care

