Hospice Visit Workflow for Comfort Care at Home
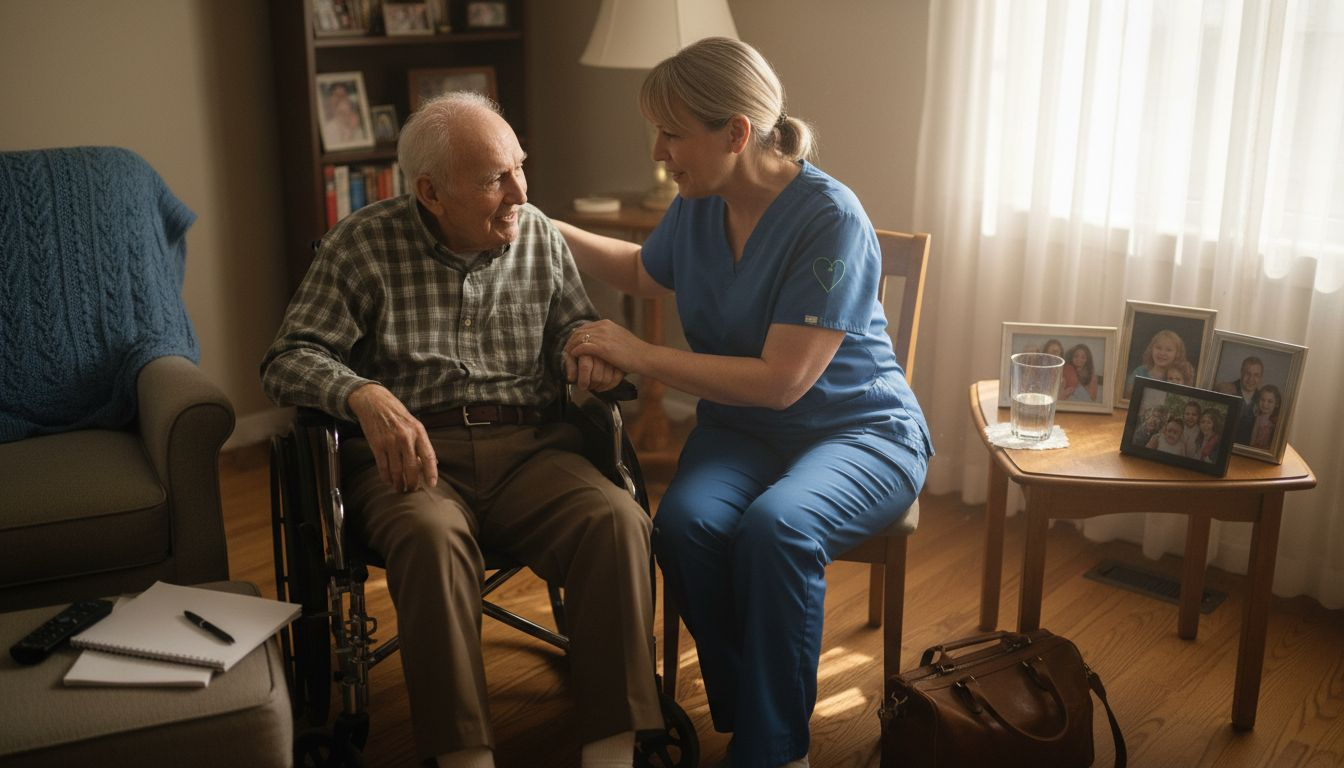
Hospice Visit Workflow for Comfort Care at Home
Caring for a terminally ill loved one at home in Orange County means facing both emotional and practical challenges. The quality of your home’s environment directly impacts patient comfort and caregiver confidence, making thoughtful preparation essential for compassionate hospice care. With a focus on patient mobility and accessibility, this guide covers clear steps for preparing your space, coordinating with hospice teams, welcoming clinicians, and supporting ongoing comfort so family caregivers can feel empowered and supported.
Table of Contents
- Step 1: Prepare the Home and Environment
- Step 2: Coordinate Visit Details with Hospice Team
- Step 3: Welcome and Support the Visiting Clinician
- Step 4: Review and Update Patient Care Plans
- Step 5: Verify Care Delivery and Ensure Comfort
- Step 6: Document the Visit and Follow Up
Quick Summary
| Important Insight | Explanation |
|---|---|
| 1. Create a Safe Home Environment | Clear pathways, install handrails, and organize spaces to enhance mobility and comfort for hospice care. |
| 2. Coordinate with Hospice Team Effectively | Establish clear communication and understand roles for more personalized, responsive comfort care during visits. |
| 3. Prepare for Clinician Visits | Ensure a welcoming space and document any observations to facilitate smooth and effective care assessments. |
| 4. Engage in Care Plan Reviews | Actively participate in discussions regarding care adjustments based on insights about symptoms and emotional needs. |
| 5. Document Each Visit Thoroughly | Maintain accurate records to support ongoing communication and adjustments in care, ensuring comprehensive support. |
Step 1: Prepare the Home and Environment
Creating a supportive home environment is crucial for providing compassionate hospice care and ensuring your loved one’s comfort and safety. Your goal is to transform your living space into a healing sanctuary that promotes physical ease and emotional well-being.
Start by conducting a comprehensive home assessment focused on patient mobility and accessibility. Creating a comfortable and supportive home care environment requires strategic modifications that reduce potential risks and enhance patient independence. Consider these essential preparations:
- Clear all walking pathways of potential tripping hazards
- Install handrails in hallways and bathrooms
- Ensure adequate lighting in all patient-used spaces
- Arrange furniture to create wide, stable movement corridors
Specifically, focus on bedroom setup as the primary care zone. An electric medical bed can provide critical positioning support and comfort for patients with limited mobility. Position the bed to maximize natural light and maintain easy access for caregivers, allowing smooth movement during care routines.
Thoughtful environmental design can significantly improve patient comfort and caregiver effectiveness.
Additionally, create dedicated spaces for medical equipment, medication management, and personal care supplies. Use labeled storage containers and maintain an organized system that allows quick access during urgent situations.

Pro tip: Photograph your room layout before making modifications, which helps you remember original configurations and can assist future care planning.
Step 2: Coordinate Visit Details with Hospice Team
Building a strong collaborative relationship with your hospice team is essential for delivering compassionate and effective comfort care for your loved one. Your primary goal is to establish clear communication channels and understand the specific roles and expectations during home hospice visits.
Effective hospice collaboration requires a structured approach to managing medical care and personal support. The hospice team will handle critical medical responsibilities, while you and your family will provide personal care and emotional support. Here are key coordination strategies:
- Schedule an initial comprehensive care planning meeting
- Discuss specific medical management protocols
- Establish preferred communication methods
- Create a backup contact list for urgent situations
- Determine visiting schedules and team member roles
During your initial meeting, focus on developing a clear communication protocol. This includes understanding how and when to report changes in your loved one’s condition, medication needs, or emotional state. Ask about the preferred contact methods - whether through phone, email, or a dedicated patient portal.
Seamless communication between family caregivers and hospice professionals ensures responsive and personalized comfort care.
Ensure you have direct contact information for each team member, including their specific roles such as nurses, counselors, and medical directors. Understand the typical response times and emergency communication procedures to feel confident and supported throughout the hospice journey.
Here’s a summary of roles in the home hospice care process:
| Role | Primary Responsibilities | Contribution to Care |
|---|---|---|
| Family Caregiver | Daily personal and emotional support | Provides continuous comfort and observation |
| Nurse | Medical oversight and symptom control | Adjusts care plan, manages medications |
| Social Worker | Resource coordination and counseling | Supports family needs and connections |
| Physician | Oversees medical direction | Confirms clinical decisions and plan changes |
| Chaplain | Spiritual, religious, and existential support | Enhances patient and family well-being |
Pro tip: Create a dedicated notebook or digital folder to track all hospice team communications, visit notes, and care instructions for easy reference and continuity.
Step 3: Welcome and Support the Visiting Clinician
Welcoming a hospice clinician into your home requires thoughtful preparation and a supportive approach that helps create a comfortable, professional environment for both the patient and healthcare provider. Your goal is to facilitate a smooth, respectful, and efficient clinical visit that prioritizes your loved one’s comfort and care needs.
Prepare for the clinician’s arrival by ensuring a welcoming and accessible care space. This involves creating an environment that allows for easy medical assessment and demonstrates your commitment to collaborative care. Consider these key preparation steps:
- Clear a direct pathway to the patient’s primary care area
- Have medical records and medication lists readily available
- Ensure good lighting and comfortable seating for the clinician
- Prepare a clean, quiet space for potential private discussions
- Have any current care concerns or observed changes documented
During the visit, focus on being an active and supportive care partner. This means listening carefully, asking thoughtful questions, and providing relevant information about your loved one’s recent health status, comfort levels, and any changes you’ve observed. Your insights can be crucial in helping the clinician understand the full context of your loved one’s condition.
A collaborative approach between family caregivers and hospice professionals creates the most effective and compassionate care environment.
Be prepared to discuss specific details such as medication effectiveness, appetite changes, sleep patterns, and emotional well-being. Offer to help position your loved one for examination if needed, and always maintain a calm, respectful demeanor that helps reduce potential stress for both the patient and clinician.
Pro tip: Keep a dedicated notebook near the patient’s care area to quickly jot down observations, questions, or care instructions immediately after the clinician’s visit.
Step 4: Review and Update Patient Care Plans
Navigating the evolving landscape of hospice care requires active engagement and consistent communication with your care team. Comprehensive hospice care planning involves a dynamic, collaborative approach that adapts to your loved one’s changing needs and ensures the highest quality of comfort and support.
Your role in the care plan review process is crucial. Understanding the care plan review process means being prepared to discuss and contribute insights about your loved one’s physical, emotional, and spiritual well-being. Key elements to focus on during care plan updates include:
- Current pain and symptom management effectiveness
- Medication response and potential adjustments
- Emotional and psychological support needs
- Functional status and mobility changes
- Spiritual and personal comfort considerations
During care plan meetings, actively participate by sharing detailed observations about your loved one’s condition. Clinical practice guidelines emphasize the importance of incorporating patient and family perspectives to create truly personalized care strategies.
Effective care planning is a collaborative journey that honors the patient’s dignity, preferences, and evolving needs.
Remember that care plans are living documents designed to provide flexible, responsive support. Be prepared to ask questions, seek clarifications, and provide honest feedback about what is working and what might need modification. Your intimate knowledge of your loved one is an invaluable resource in tailoring their hospice care experience.
Pro tip: Create a dedicated digital or physical folder to track each care plan version, noting dates of updates and key discussion points for future reference.
Step 5: Verify Care Delivery and Ensure Comfort
Ensuring your loved one receives compassionate, high-quality hospice care requires active engagement and careful monitoring. Hospice care overview emphasizes the critical role families play in supporting comfort and dignity during this sensitive journey.
Your primary focus should be on monitoring care quality and patient comfort. This involves systematic observation and communication with the hospice team about your loved one’s physical and emotional well-being. Key verification strategies include:
- Track medication effectiveness and symptom management
- Observe patient’s pain levels and comfort
- Monitor emotional and psychological responses
- Assess mobility and physical support needs
- Verify equipment functionality and appropriateness
During each hospice visit, engage actively by asking specific questions about care delivery. Pay attention to how interventions are implemented, watch for subtle changes in your loved one’s condition, and be prepared to provide detailed feedback to the care team.
Compassionate care is a collaborative process that requires ongoing communication, observation, and mutual respect.
Remember that comfort goes beyond physical symptoms. It encompasses emotional, spiritual, and psychological well-being. Be attentive to your loved one’s nonverbal cues, mood changes, and overall sense of peace. Your intuitive understanding combined with professional hospice expertise creates a holistic care environment.
Pro tip: Maintain a daily care journal documenting observations, medication responses, and emotional states to provide comprehensive insights during team consultations.
Step 6: Document the Visit and Follow Up
Documenting each hospice visit is a critical step in ensuring comprehensive, continuous care for your loved one. Hospice nursing documentation plays a vital role in tracking patient progress, managing symptoms, and maintaining clear communication across the care team.
Your documentation should focus on capturing comprehensive visit details with precision and clarity. Key elements to record include:
- Specific symptoms and their intensity
- Medication effectiveness and responses
- Changes in physical or cognitive status
- Emotional and psychological observations
- Any concerns raised during the visit
- Interventions performed and their immediate impact
Create a systematic approach to tracking information. Use a dedicated notebook or digital app to ensure you capture important care details consistently. This documentation becomes an invaluable resource for the hospice team, helping them adjust care plans and respond quickly to changing needs.
Accurate and thorough documentation bridges communication gaps and supports personalized, responsive care.
Remember that your observations are crucial. Healthcare professionals rely on family insights to understand the patient’s condition between formal assessments. Be specific, objective, and timely in your notes, focusing on observable changes and notable interactions.
Pro tip: Take brief notes immediately after each visit while details are fresh, then transfer to a more organized format within 24 hours to maintain accuracy and completeness.
Compare routine hospice visit elements with follow-up responsibilities:
| Step | During Visit | After Visit |
|---|---|---|
| Monitoring | Check symptoms and status with team | Review notes and provide updates |
| Communication | Discuss changes with clinicians | Share updates, ask further questions |
| Documentation | Record specific interventions | Log details promptly and organize records |
| Adjustment | Recommend immediate changes | Evaluate long-term effectiveness, feedback |
| Emotional Support | Offer real-time reassurance | Continue support between visits |
Enhance Comfort Care at Home with Expert Support
Navigating the complexities of hospice visit workflow for comfort care at home can feel overwhelming. From preparing a safe environment to coordinating closely with hospice clinicians and reviewing care plans, each step demands attention to detail and compassionate engagement. At Graceland Hospice, we understand these challenges and the critical need for seamless communication, thorough documentation, and personalized care strategies that honor your loved one’s dignity and evolving needs.
Let us help you transform your home care experience by providing reliable hospice expertise and heartfelt support. Discover practical solutions for managing every stage of hospice visits—from welcoming clinicians to verifying comfort and updating care plans—while feeling empowered as the central caregiver. Explore resources and learn how we set the gold standard in compassionate hospice care by visiting our blog at Graceland Hospice Blog. Take the first step toward elevating your loved one’s comfort today by contacting us for a free consultation at https://gracelandhc.com/blog.
Experience the difference of care delivered with passion and excellence tailored to the sensitive journey of home hospice. Start your path to peace of mind now.
Frequently Asked Questions
How can I prepare my home environment for hospice visits?
Creating a supportive home environment begins with conducting a comprehensive home assessment. Ensure that all walking pathways are clear, install handrails as needed, and arrange furniture to allow easy movement for both your loved one and the hospice clinician.
What should I discuss during the initial meeting with the hospice team?
During the initial meeting, focus on discussing specific medical management protocols, preferred communication methods, and the roles of each hospice team member. Establishing a clear communication protocol will help ensure that everyone understands how to report changes in your loved one’s condition.
How can I actively support my loved one during hospice visits?
Be an active participant by listening carefully to the clinician and providing relevant information about your loved one’s recent health status. Taking notes on any observed changes and asking thoughtful questions will help facilitate a productive visit for both the patient and the healthcare provider.
What details should I document after each hospice visit?
Document key details such as symptoms and their intensity, medication effectiveness, and changes in physical or emotional states. This documentation should be concise and organized, capturing essential information that can help the hospice team adjust care plans as needed.
How often should I review and update the patient care plan?
You should review and update the patient care plan regularly—ideally at least once a month or whenever there are significant changes in your loved one’s condition. Actively participating in care plan meetings and sharing your observations will ensure the care plan remains tailored to your loved one’s evolving needs.
What strategies can help verify the quality of hospice care delivered at home?
To verify care quality, track your loved one’s medication effectiveness, monitor their comfort levels, and communicate any concerns with the hospice team. Engaging actively in this way will help ensure that both physical and emotional well-being are being addressed effectively.
Recommended
- Graceland Hospice Care | Compassionate End-of-Life Care
- Graceland Hospice Care | Compassionate End-of-Life Care
- Graceland Hospice Care | Compassionate End-of-Life Care
- Graceland Hospice Care | Compassionate End-of-Life Care
- Role of Caregivers in Hearing Aid Choice – Impact on Elderly Wellbeing – Audora

