Effective communication strategies for end-of-life care

Effective communication strategies for end-of-life care
Many families believe talking about end-of-life care is taboo or too emotionally difficult to approach. This misconception keeps loved ones from having crucial conversations that could ease anxiety and improve care quality. Research demonstrates that early conversations reduce anxiety and hospitalizations, significantly enhancing quality of life for patients and caregivers. This guide provides practical, compassionate strategies to help you navigate these vital discussions with confidence, ensuring your loved one’s wishes are honored and understood.
Table of Contents
- Key takeaways
- Why early and compassionate communication matters
- Core strategies and frameworks for effective communication
- Addressing cultural sensitivity and caregiver involvement
- Practical tips for families navigating end-of-life conversations at home
- Explore compassionate hospice care services
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Early conversations reduce anxiety | Starting these conversations early can lower anxiety and reduce unnecessary hospitalizations, leading to better quality of life for patients and families. |
| Clear compassionate language | Use simple language that avoids medical jargon so loved ones understand goals and options without confusion. |
| Ask Tell Ask method | The ask tell ask approach invites input by asking what is known, providing clear information, and checking understanding. |
| SPIKES protocol | The SPIKES framework provides a six step process for delivering difficult news with empathy. |
Why early and compassionate communication matters
Starting end-of-life conversations before crisis situations emerge helps reduce stress for everyone involved. When families wait until emergencies force these discussions, emotions run high and decision-making becomes rushed and overwhelming. Patients and families consistently report higher satisfaction when prognosis and care goals are discussed timely, allowing thoughtful planning rather than reactive choices.
Several barriers prevent these important conversations from happening. Cultural stigma around death makes many people uncomfortable acknowledging mortality, even when a loved one faces serious illness. Healthcare system fragmentation compounds this challenge, as stigma and fragmented systems complicate communication between providers, patients, and families. Without coordinated care, critical information gets lost and conversations fall through the cracks.
Educating caregivers and families about communication benefits breaks down these barriers effectively. When people understand that honest discussions actually reduce suffering rather than cause it, they feel more prepared to engage. Supporting caregivers with proper resources and training improves their ability to facilitate meaningful conversations and advocate for their loved ones.
“Open communication about prognosis and preferences transforms end-of-life care from crisis management to compassionate planning that honors patient wishes and reduces family distress.”
Key benefits of early communication include:
- Reduced emergency hospitalizations and invasive interventions
- Better alignment between care received and patient preferences
- Lower anxiety levels for both patients and family members
- Improved symptom management through proactive planning
- Stronger family relationships during difficult times
Families who engage in caregiver support in hospice programs report feeling more confident and less isolated. These resources provide practical guidance on initiating conversations, understanding medical information, and managing the emotional weight of caregiving responsibilities.
Core strategies and frameworks for effective communication
Creating the right environment sets the foundation for productive conversations. Choose a quiet, private space free from distractions where everyone feels comfortable speaking openly. Turn off phones and televisions, and ensure adequate time so no one feels rushed. Physical comfort matters too, so arrange seating that allows eye contact without feeling confrontational.

Use simple, jargon-free language that respects your loved one’s intelligence while ensuring clarity. Medical terminology confuses people and creates distance when you need connection. Instead of saying “palliative interventions,” say “treatments focused on comfort.” This compassionate approach makes information accessible and reduces anxiety.
The ask-tell-ask method creates dialogue rather than monologue:
- Ask what the person already knows or wants to know
- Tell them information clearly and simply
- Ask what they understood and how they feel about it
This technique checks understanding continuously and invites input, making the person an active participant rather than a passive recipient of information.
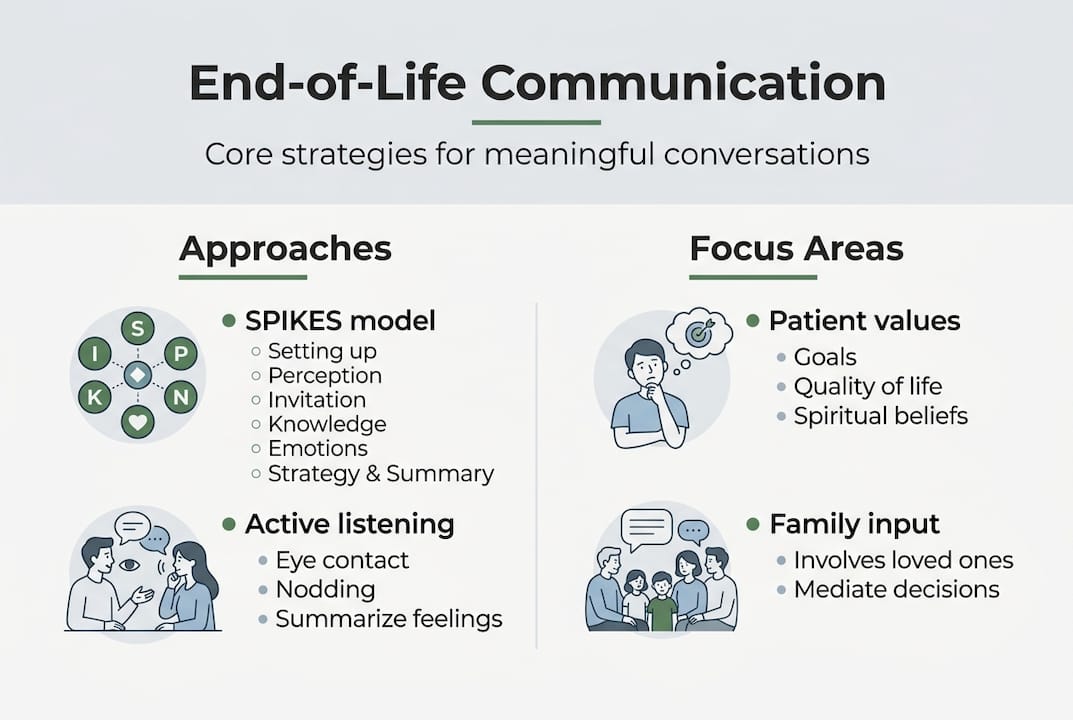
The SPIKES protocol guides breaking bad news through six steps: Setting, Perception, Invitation, Knowledge, Emotions, and Strategy/Summary. Each step builds on the previous one, creating a compassionate framework that acknowledges feelings while delivering necessary information. This structured approach prevents overwhelming people with too much information at once.
Goals of Care Conversations shift focus from medical procedures to patient values and preferences. Instead of asking “Do you want CPR?” ask “What matters most to you as your health changes?” This reframing helps families understand the purpose behind medical decisions and ensures care aligns with deeply held values.
Pro Tip: Keep an end-of-life care checklist handy during conversations to ensure you cover important topics without forgetting crucial details in emotional moments.
| Communication approach | Best used when | Key benefit |
|---|---|---|
| SPIKES framework | Delivering difficult news or diagnosis | Structures emotional conversations with empathy |
| Goals of Care | Planning treatment direction | Aligns medical care with patient values |
| Ask-tell-ask method | Sharing any medical information | Ensures understanding and invites participation |
| Open-ended questions | Beginning conversations | Encourages dialogue and reveals concerns |
Healthcare professionals trained in these methods report more satisfying interactions with families. The qualities of hospice staff include excellent communication skills precisely because these conversations require both technical knowledge and emotional intelligence.
Addressing cultural sensitivity and caregiver involvement
Respecting cultural beliefs shapes more effective and respectful communication across diverse communities. Different cultures hold varying views about discussing death, family decision-making authority, and appropriate care at life’s end. Some traditions emphasize protecting patients from distressing news, while others prioritize individual autonomy and full disclosure.
Avoid medical jargon and tailor language to each individual’s cultural context and communication preferences. What works for one family may not resonate with another. Some cultures prefer indirect communication about serious topics, using metaphors or discussing possibilities rather than certainties. Others value direct, factual information delivered plainly.
Active listening and soliciting patient input adapt beautifully across cultural and personal differences. Asking “What would be most helpful for you right now?” or “How does your family usually handle important health decisions?” demonstrates respect and gathers crucial information about preferences.
Caregiver-centered communication approaches improve involvement and satisfaction significantly. When healthcare providers actively engage family caregivers as partners rather than bystanders, everyone benefits. Caregivers gain confidence in their abilities, patients receive more coordinated care, and families feel valued and heard.
Key cultural sensitivity practices include:
- Asking about religious or spiritual beliefs that influence care preferences
- Identifying who should be included in important conversations
- Respecting different communication styles and pacing
- Acknowledging that silence can be meaningful and appropriate
- Offering interpreter services when language barriers exist
Ongoing training for providers enhances sensitivity and competence in diverse settings. The role of caregivers in hospice extends beyond physical care to cultural liaison, helping professional teams understand family dynamics and preferences.
Pro Tip: When supporting a loved one through end-of-life care, ask early in the relationship about cultural or religious practices that should guide care decisions, then document these preferences clearly.
Caregivers often navigate between medical systems and family expectations, translating not just language but cultural concepts. Recognizing this vital role and supporting caregivers with resources, education, and emotional support strengthens the entire care network.
Practical tips for families navigating end-of-life conversations at home
Preparing for conversations increases confidence and effectiveness. Choose an appropriate time when everyone feels relatively calm and unhurried, not immediately after receiving difficult news or during medical crises. A quiet space at home, perhaps around the kitchen table or in a comfortable living room, often works better than a hospital setting.
Follow these steps for successful home conversations:
- Express your love and concern first, establishing emotional safety
- Invite the person to share their thoughts and feelings without judgment
- Share information clearly using simple language they understand
- Pause frequently to check comprehension and emotional state
- Document important preferences and decisions together
- Plan to revisit the conversation as situations or feelings change
Use clear, simple language and check for understanding regularly throughout the discussion. Phrases like “Does this make sense?” or “What questions do you have?” create openings for clarification. Remember that people often need to hear information multiple times, especially when processing emotional content.
Encourage shared decision-making by asking what matters most to your loved one. Listen empathetically without interrupting or rushing to solutions. Sometimes people need to express fears or sadness before they can engage with practical planning.
Be patient with emotions like denial or fear, which are normal protective responses to difficult realities. Pushing too hard can damage trust and shut down communication. If someone isn’t ready to discuss certain topics, respect that boundary while gently keeping the door open for future conversations.
“Effective home communication balances honesty with hope, providing clear information while honoring each person’s emotional readiness and cultural values.”
Seek professional hospice support for guidance and additional resources when conversations feel overwhelming. Trained hospice professionals bring expertise in facilitating difficult discussions and can mediate family disagreements or clarify medical information. Structured communication improves caregiver involvement and reduces anxiety in home hospice settings significantly.
Common challenges and solutions include:
- Challenge: Family members disagree about care approaches. Solution: Facilitate a family meeting with a hospice professional to find common ground.
- Challenge: Your loved one changes their mind about preferences. Solution: Revisit conversations regularly and update documentation as wishes evolve.
- Challenge: You feel too emotional to have difficult conversations. Solution: Ask a trusted friend, family member, or hospice counselor to facilitate.
- Challenge: Medical information feels overwhelming and confusing. Solution: Request that healthcare providers explain concepts simply and provide written summaries.
Understanding the hospice visit workflow helps families know what to expect and when opportunities for important conversations naturally arise. Regular hospice visits create ongoing touchpoints for discussing changes in condition, adjusting care plans, and addressing new concerns.
The end-of-life care at home guide provides comprehensive information about managing physical symptoms, emotional support, and practical logistics, complementing the communication strategies outlined here.
Explore compassionate hospice care services
Navigating end-of-life communication and care planning can feel overwhelming, but you don’t have to do it alone. Graceland Hospice Care offers professional, compassionate hospice services tailored specifically to home care needs throughout Southern California. Our experienced team supports families with communication guidance, symptom management, and emotional comfort during this critical time.
We understand that effective communication forms the foundation of quality end-of-life care. Our caregivers receive extensive training in the frameworks and cultural sensitivity approaches discussed in this guide. When you partner with Graceland, you access expert professionals who know how to facilitate difficult conversations, honor patient wishes, and support entire families through the hospice journey.
Explore our compassionate hospice care approach and learn how we tailor services to each family’s unique needs. Our comprehensive hospice care services include medical care, emotional support, spiritual counseling, and caregiver education. Families throughout the region trust hospice care in Orange County to provide dignified, personalized support when it matters most. Contact us today for a free consultation.
Frequently asked questions
How can I start a conversation about end-of-life wishes with a loved one?
Choose a quiet, private moment when you both feel calm and unhurried. Express your concern and love first, then use open-ended questions like “Have you thought about what matters most to you as your health changes?” to invite dialogue. Listen attentively without judgment, allowing your loved one to guide the conversation’s pace and depth.
What if my loved one avoids talking about their prognosis?
Respect their feelings and give them space rather than forcing the conversation. Avoidance often reflects fear, denial, or cultural beliefs about discussing death. Find gentle ways to revisit the topic over time, perhaps through smaller questions about immediate comfort preferences. Engage professional hospice support if persistent avoidance prevents necessary care planning.
How can I balance hope and honesty in end-of-life communication?
Use compassionate language that acknowledges feelings while sharing clear information about the situation. Hope doesn’t require denying reality; it can focus on comfort, quality time together, and honoring wishes. Employ frameworks like ask-tell-ask to check understanding and adjust your message based on what the person wants to know and can process emotionally.
Where can I find professional help for end-of-life communication challenges?
Hospice providers like Graceland offer trained staff specifically prepared to assist with communication and care planning challenges. Our team facilitates family meetings, clarifies medical information, and mediates disagreements with compassion and expertise. Look for local hospice care services in your community, and don’t hesitate to request communication support as part of comprehensive hospice care.
Recommended
- Supporting a Loved One Through End-of-Life Care | Graceland Hospice Care Blog
- 7 Essential Steps in an End of Life Care Checklist for Caregivers | Graceland Hospice Care Blog
- End of Life Care Guide for Compassionate At-Home Support | Graceland Hospice Care Blog
- Caregiver Support in Hospice: Easing End-of-Life Care | Graceland Hospice Care Blog
- Signs It’s Time for an Elderly Care Plan | Senior Concierge

